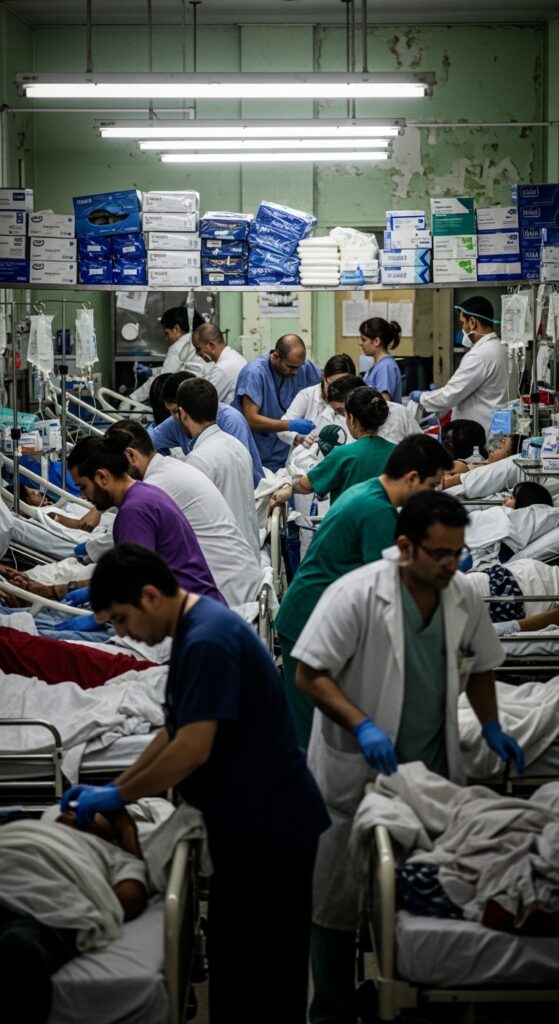
From conflict zones to disease outbreaks, health systems are being tested by shrinking funds and rising humanitarian needs.
Global health agencies are warning that emergencies are stretching medical response systems beyond sustainable limits. Conflicts, displacement, disease outbreaks and climate-related disasters are arriving simultaneously, often in places where hospitals and clinics were already fragile.
The World Health Organization’s 2026 emergency appeal says more than 239 million people need urgent humanitarian assistance. The agency is seeking about $1 billion to maintain life-saving care in severe emergencies, including vaccination, disease surveillance, trauma care, maternal health and support for damaged health systems.
The scale of need reflects a world where health crises rarely occur alone. A conflict can destroy clinics and force people into crowded shelters, where infectious diseases spread more easily. A flood can contaminate water and interrupt medicine supply chains. A drought can worsen malnutrition and make children more vulnerable to disease.
Vaccination remains a central line of defense. When routine immunization collapses, diseases that were controlled can return. Catch-up campaigns are therefore not only medical operations but acts of crisis prevention. They require cold chains, trained workers, community trust and secure access.
Disease surveillance is equally important. Early detection can prevent an outbreak from becoming a regional emergency. But surveillance depends on laboratories, reporting systems and local health workers. In unstable settings, those systems are often damaged or underfunded.
Health workers are under extreme pressure. Doctors, nurses, midwives and community workers continue providing care despite shortages, insecurity and exhaustion. In some places, they work without reliable electricity, clean water or essential medicines. Their resilience is often praised, but praise does not replace funding or protection.
Mental health is increasingly recognized as part of emergency response. War, displacement, bereavement and disaster leave psychological wounds that can last for years. Emergency medicine must treat trauma, infection and childbirth, but it must also support people living with fear and loss.
The funding gap forces hard choices. Agencies may focus on the most immediate life-saving services while cutting prevention, rehabilitation or long-term support. That approach can save lives in the short term but leave communities vulnerable to the next crisis.
Public trust is another challenge. In emergencies, misinformation can spread quickly. Communities may distrust outside agencies or government authorities. Effective health response depends on local partnerships, clear communication and respect for culture.
The broader lesson is that health security cannot be separated from political stability, climate resilience and development. A hospital can treat injuries, but it cannot stop a war. A vaccination campaign can prevent disease, but it cannot fully protect children living without clean water.
The world has the medical knowledge to prevent many deaths in emergencies. What it often lacks is access, funding and political will. In 2026, global health will be judged not by scientific capacity alone, but by whether that capacity reaches people in the hardest places.”””